Australian survey to shed light on treating herpes "down under"

Have your say on treating genital herpes
Australians living with the nation's second most common sexually transmitted infection (STI) are being urged to convey their experience and challenges by completing a new online survey.
The Australian Herpes Management Forum (AHMF) is calling for people who have been diagnosed with and treated for genital herpes to participate in the Genital Herpes Patient Perspectives Survey of herpes management and treatment practices.
The survey, located at ahmf.com.au/herpes-treatment-survey, will provide an up-to-date snapshot of the views of Australians living with genital herpes.
According to leading infectious disease expert, Professor Tony Cunningham, Director of the Westmead Millennium Institute and Research Centre, Westmead Hospital, Sydney, the online survey has been designed to improve clinical understanding of patient experiences and thoughts on the most effective treatments available for genital herpes.
"Gathering Australian-specific information about current experiences with treatment will allow the healthcare community to respond directly to the needs and concerns of people living with genital herpes.
"It is important that people with genital herpes understand the treatment options available and can evaluate which option is best for them, particularly given that 12 per cent of Australians over the age of 25 are carrying the virus,"1 said Prof Cunningham.
All survey respondents will be canvassed on their diagnosis and treatment experience. In particular, they will be asked for their thoughts on episodic treatment [treating the genital herpes outbreaks as they occur] and suppressive treatment [taking daily medication to reduce the chance of an outbreak occurring].2 The information provided by all survey respondents will remain strictly anonymous.
One-in-eight Australians has genital herpes.1 Evidence suggests that the incidence of genital herpes in Australia is increasing, particularly among Gen Y.3 An Australian online survey, conducted in 2006-2007 that assessed a person's risk of contracting genital herpes, revealed that 51 per cent of survey participants were at "medium" risk of contracting the genital herpes virus, while 34 per cent were at "high" risk.4
Given that genital herpes is generally transmitted through skin-to-skin contact, most commonly through sexual contact, the virus can spread easily from person-to-person. While some people with genital herpes have no noticeable symptoms, others can experience their first outbreak two-to-20 days after coming into contact with the virus.5
"Most of the time, the genital herpes virus lies inactive and often without symptoms. When re-activated, the virus travels down the nerve paths to the surface of the skin, causing an outbreak,"6 said Prof Cunningham.
"Even after the first outbreak of genital herpes, the virus stays in the body for life.6
"It is possible to pass on the virus, with or without symptoms,"5 Prof Cunningham said.
"While there is currently no cure for genital herpes, providing effective, patient-friendly management and treatment options is essential to supporting those living with the virus."
To participate in the Genital Herpes Patient Perspectives Survey, go to ahmf.com.au/herpes-treatment-survey.
The Australian Herpes Management Forum (AHMF) is calling for people who have been diagnosed with and treated for genital herpes to participate in the Genital Herpes Patient Perspectives Survey of herpes management and treatment practices.
The survey, located at ahmf.com.au/herpes-treatment-survey, will provide an up-to-date snapshot of the views of Australians living with genital herpes.
According to leading infectious disease expert, Professor Tony Cunningham, Director of the Westmead Millennium Institute and Research Centre, Westmead Hospital, Sydney, the online survey has been designed to improve clinical understanding of patient experiences and thoughts on the most effective treatments available for genital herpes.
"Gathering Australian-specific information about current experiences with treatment will allow the healthcare community to respond directly to the needs and concerns of people living with genital herpes.
"It is important that people with genital herpes understand the treatment options available and can evaluate which option is best for them, particularly given that 12 per cent of Australians over the age of 25 are carrying the virus,"1 said Prof Cunningham.
All survey respondents will be canvassed on their diagnosis and treatment experience. In particular, they will be asked for their thoughts on episodic treatment [treating the genital herpes outbreaks as they occur] and suppressive treatment [taking daily medication to reduce the chance of an outbreak occurring].2 The information provided by all survey respondents will remain strictly anonymous.
One-in-eight Australians has genital herpes.1 Evidence suggests that the incidence of genital herpes in Australia is increasing, particularly among Gen Y.3 An Australian online survey, conducted in 2006-2007 that assessed a person's risk of contracting genital herpes, revealed that 51 per cent of survey participants were at "medium" risk of contracting the genital herpes virus, while 34 per cent were at "high" risk.4
Given that genital herpes is generally transmitted through skin-to-skin contact, most commonly through sexual contact, the virus can spread easily from person-to-person. While some people with genital herpes have no noticeable symptoms, others can experience their first outbreak two-to-20 days after coming into contact with the virus.5
"Most of the time, the genital herpes virus lies inactive and often without symptoms. When re-activated, the virus travels down the nerve paths to the surface of the skin, causing an outbreak,"6 said Prof Cunningham.
"Even after the first outbreak of genital herpes, the virus stays in the body for life.6
"It is possible to pass on the virus, with or without symptoms,"5 Prof Cunningham said.
"While there is currently no cure for genital herpes, providing effective, patient-friendly management and treatment options is essential to supporting those living with the virus."
To participate in the Genital Herpes Patient Perspectives Survey, go to ahmf.com.au/herpes-treatment-survey.
References
1 Cunningham AL, Taylor R, Taylor J, Marks C, Shaw J, Mindel A. Prevalence of infection with herpes simplex virus types 1 and 2 in Australia: a nationwide population based survey. Sex Transm Infect 2006; 82: 164-168.
2 Australian Herpes Management Forum. Guidelines for clinicians: Managing genital herpes [fact sheet]. Feb 2008.
3 Australian Government Department of Health and Ageing. National Sexually Transmissible Infections Strategy 2005-2008. 2005; Publication 3681.
4 Mindel A, McHugh L, Christie E, Chung C, Berger T and the AHMF. Genital Herpes - An internet-based risk survey. Int J STD AIDS 2009 (In press).
5 Ooi, C & Dayan, L. Genital herpes: an approach for general practitioners in Australia. Australian Family Physician 2002; 31:9.
6 Sacks, SL. The truth about herpes. 1997 4th Edition, Gordon Soules Book Publishers Ltd, West Vancouver, Canada.
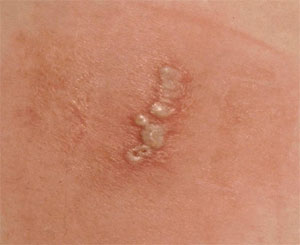
All about genital herpes
What is genital herpes?
- Genital herpes is a common infection caused by the herpes simplex virus, HSV-1 and HSV-2.1
- HSV-1 most commonly causes cold sores, but can also be transmitted to the genitals through direct skin-to-skin contact, often via oral sex. About 80 per cent of adults have HSV-1.1
- HSV-2 is responsible for most genital herpes and is commonly transmitted through sexual contact.1
- Approximately one-in-eight active Australians over the age of 25 has HSV-2.2 Of these, 20 per cent are aware that they have the virus, 60 per cent are unaware that they have it, but have symptoms, while another 20 per cent have no symptoms.3
Transmission of the virus
- Genital herpes is transmitted through skin-to-skin contact or sexual contact.1
- This may occur when a person has a recurrence, but it more commonly it occurs between episodes, when the virus is still found on the skin, but there are no symptoms.4
- Twenty per cent of people who have been exposed to HSV-1 or HSV-2 never develop any symptoms.3 Even without symptoms, these people are infectious and can transmit the infection at any time.4
Symptoms
- The first symptoms of genital herpes may occur two-to-20 days after first contact with the virus.5
- This first episode of genital herpes is often the most severe because the immune system has not had time to develop antibodies to protect against the virus.1
- Symptoms may include swollen lymph nodes (glands in the groin, neck and armpit), or flu-like symptoms (sore muscles, tiredness, headaches, fever and chills).1
- Other symptoms can include swelling, pain or itching around the genitals, possibly followed by painful red spots that can form small blisters. These blisters may burst to form open sores or ulcers, which crust over and heal. There may also be pain during urination.1
- Usually symptoms associated with the first episode heal in a few weeks.1
- Following the first episode, 95 per cent of individuals will have recurrences of the infection.6
- These are usually mild and short lived. Most people with herpes only have occasional recurrences, but some will have then every month or even more often.1
Treatment
- Treatments for genital herpes can reduce the severity, frequency and duration of outbreaks.5
- There are currently 3 herpes antiviral medications available in tablet form - famciclovir, aciclovir and valaciclovir.5
- Antiviral medications help stop the virus from multiplying, effectively reducing the duration of outbreaks.1
- Genital herpes may be treated episodically or suppressively.5
- Episodic treatment involves treating each recurrence when it occurs.5
- Taking a two-day or a five-day episodic treatment at the first signs of an outbreak will help reduce the length and severity of symptoms.5
- Suppressive (preventative) treatment involves taking medication on a daily basis to reduce the chance of an outbreak occurring.5
- Continuous suppressive treatment is useful for those who are experiencing frequent recurrences. Most individuals taking suppressive treatment will either have no recurrences or very few minor episodes during treatment.5
More information available from www.herpes.com.au
- Genital herpes is a common infection caused by the herpes simplex virus, HSV-1 and HSV-2.1
- HSV-1 most commonly causes cold sores, but can also be transmitted to the genitals through direct skin-to-skin contact, often via oral sex. About 80 per cent of adults have HSV-1.1
- HSV-2 is responsible for most genital herpes and is commonly transmitted through sexual contact.1
- Approximately one-in-eight active Australians over the age of 25 has HSV-2.2 Of these, 20 per cent are aware that they have the virus, 60 per cent are unaware that they have it, but have symptoms, while another 20 per cent have no symptoms.3
Transmission of the virus
- Genital herpes is transmitted through skin-to-skin contact or sexual contact.1
- This may occur when a person has a recurrence, but it more commonly it occurs between episodes, when the virus is still found on the skin, but there are no symptoms.4
- Twenty per cent of people who have been exposed to HSV-1 or HSV-2 never develop any symptoms.3 Even without symptoms, these people are infectious and can transmit the infection at any time.4
Symptoms
- The first symptoms of genital herpes may occur two-to-20 days after first contact with the virus.5
- This first episode of genital herpes is often the most severe because the immune system has not had time to develop antibodies to protect against the virus.1
- Symptoms may include swollen lymph nodes (glands in the groin, neck and armpit), or flu-like symptoms (sore muscles, tiredness, headaches, fever and chills).1
- Other symptoms can include swelling, pain or itching around the genitals, possibly followed by painful red spots that can form small blisters. These blisters may burst to form open sores or ulcers, which crust over and heal. There may also be pain during urination.1
- Usually symptoms associated with the first episode heal in a few weeks.1
- Following the first episode, 95 per cent of individuals will have recurrences of the infection.6
- These are usually mild and short lived. Most people with herpes only have occasional recurrences, but some will have then every month or even more often.1
Treatment
- Treatments for genital herpes can reduce the severity, frequency and duration of outbreaks.5
- There are currently 3 herpes antiviral medications available in tablet form - famciclovir, aciclovir and valaciclovir.5
- Antiviral medications help stop the virus from multiplying, effectively reducing the duration of outbreaks.1
- Genital herpes may be treated episodically or suppressively.5
- Episodic treatment involves treating each recurrence when it occurs.5
- Taking a two-day or a five-day episodic treatment at the first signs of an outbreak will help reduce the length and severity of symptoms.5
- Suppressive (preventative) treatment involves taking medication on a daily basis to reduce the chance of an outbreak occurring.5
- Continuous suppressive treatment is useful for those who are experiencing frequent recurrences. Most individuals taking suppressive treatment will either have no recurrences or very few minor episodes during treatment.5
More information available from www.herpes.com.au
References
1 Sacks SL. The truth about herpes. 1997 4th Edition, Gordon Soules Book Publishers Ltd, West Vancouver, Canada.
2 Cunningham AL, Taylor R, Taylor J, Marks C, Shaw J, Mindel A. Prevalence of infection with herpes simplex virus types 1 and 2 in Australia: a nationwide population based survey. Sex Transm Infect 2006; 82: 164-168.
3 Australian Herpes Management Forum. Guidelines for clinicians: Managing genital herpes [fact sheet]. Feb 2008.
4 Mertz GJ, Benedetti J, Ashley R, Selke SA, Corey L. Risk factors for the sexual transmission of genital herpes. Ann Int Med 1992; 116(3): 197-202.
5 Ooi C & Dayan L. Genital herpes: an approach for general practitioners in Australia. Australian Family Physician 2002; 31:9.
6 Australian Herpes Management Forum. Guidelines for clinicians: Suppressive therapy for genital herpes [fact sheet]. Apr 2008.
MORE
- Cold Sores
- Glandular Fever
- FAQ About Irritable Bowel Syndrome
- February is Ovarian Cancer Awareness Month
- Help find answers for Herpes
- National Eczema Awareness Week
- Claire Naffah It's Dementia
- Skin Cancer and Melanoma
- Treatment for Early-stage Breast Cancer
- Structured Reporting for Cancer Patients
- Tuberculosis



